COPD vs. Bronchiectasis

Chronic obstructive pulmonary disease (COPD) and bronchiectasis are two chronic lung conditions. They have similar symptoms and their causes are rooted in roughly the same anatomical features. Nonetheless, COPD and bronchiectasis are very different diseases requiring two different means of treatment. Here’s a look at COPD, bronchiectasis, and the differences between the two.
What is COPD?
Put simply: COPD makes it difficult to breathe. The most common cause of COPD is smoking. The bronchioles and alveoli (air sacs on the branches of the bronchioles) lose their elasticity, making it difficult to breathe. In particular, it becomes difficult to push air back out of your lungs, which means no complete round of reoxygenation for your blood.
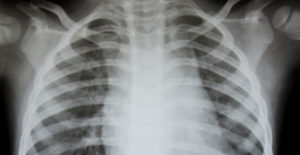
Pulmonary function tests are an important part of diagnosing chronic obstructive pulmonary disease. The most common test is spirometry, which involves blowing into a device called a spirometer, which then measures the air your lungs can hold and how fast you can expel that air. Additional diagnostic methods include a chest x-ray, CT scan, and other tests.
According to the Mayo Clinic, symptoms of COPD include shortness of breath, wheezing, tightness in the chest, and fatigue. You may also produce excess mucus, especially after waking up, which comes up from the persistent cough that accompanies COPD. Having COPD may make you more susceptible to respiratory illnesses. As the disease progresses, you may notice areas like your nail beds becoming blue from too little oxygen, swollen ankles and feet, and inadvertent weight loss.
The most important treatment is to quit smoking cigarettes. Pharmaceutical treatment for COPD requires a combination of medications. You may require multiple inhalers; bronchodilators help the airways stay open and inhaled steroids reduce inflammation. There are some inhalers available, like Advair and Symbicort, that deliver a combination of the medications. Oral steroids, theophylline, and new medications, such as phosphodiesterase-4 inhibitors, also help improve quality of life.
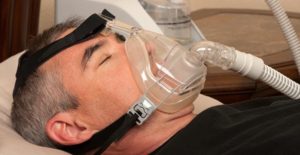
Sufferers of moderate to severe COPD may also need supplemental oxygen therapies.
What is Bronchiectasis?
Bronchiectasis is another chronic lung disorder characterized by a thickness of the bronchial walls, generally as a result of inflammation or infections. It usually develops as a result of systemic illnesses, most commonly cystic fibrosis.
Symptoms of bronchiectasis include the persistent expulsion of yellow or green mucus and a shortness of breath during exacerbations (periods when the disease flares up and makes breathing more difficult). Other symptoms include wheezing, whistling breaths, and blood mixed with sputum. Additionally, you may notice fatigue, a fever, or chills, especially during exacerbations.
Treatment involves antibiotics to get rid of any bacteria that may be causing thickening, particularly a specific type of antibiotic called “macrolides.” It can also be helpful to use medications or products that thin mucus like mucolytics or expectorants, making it easier to cough up.
What’s the Difference?
The biggest difference between COPD and bronchiectasis is that COPD is almost completely preventable by not smoking. On the other hand bronchiectasis can pop up because of unavoidable underlying diseases. Symptomatically, although similar, there are a few distinctions.
While bronchiectasis may be a dry or wet cough with yellow or green mucus only, COPD is generally a wet cough and sputum may be clear or white in addition to yellow or green. Although both are pulmonary disorders, COPD is rooted in the elasticity of the alveoles while bronchiectasis is rooted in thick bronchi. Of course, the courses of treatment required for these diseases are very different. If you suspect you have a chronic lung condition, talk to your doctor about treatment options as soon as possible.